By DR. Richard Bosshardt
The Most Common Cancers
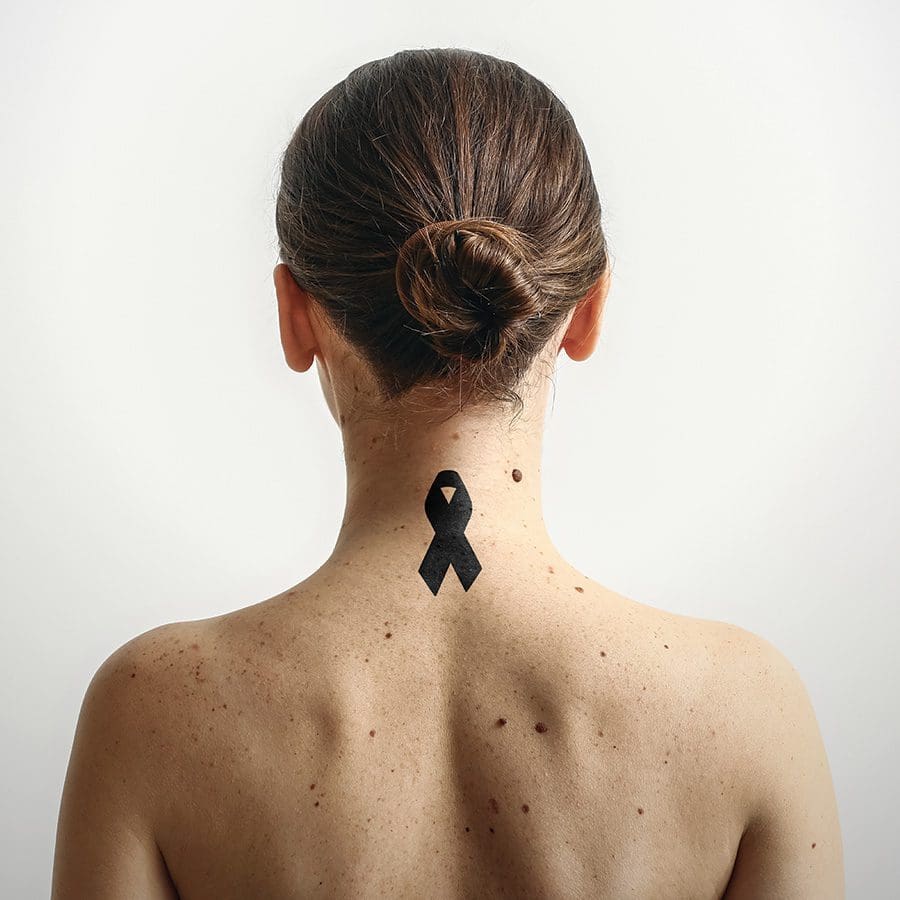
The best biopsy for melanoma
Save your skin and possibly your life.
Skin cancers are the most common cancers, and even though only about 1% of skin cancers are melanoma, it is the one that concerns physicians—and should concern most patients—because it can be lethal.
Melanomas do not always appear as the classic large, irregular, very dark to black mole. They can be brown, blue, red, and even non-pigmented, thus evading detection until very advanced. With appearance sometimes a bit equivocal, often the only way to make this diagnosis for sure is by taking a biopsy (a piece) of the mole to be examined microscopically for cancer cells.
There are several ways a biopsy can be taken. If the mole or lesion is very small, an excisional biopsy can be performed and entails the removal of the entire mole. Even if the examination proves that the entire melanoma was removed, this is rarely sufficient. Melanomas need to be taken with a generous margin of skin, but that isn’t done until the diagnosis justifying extensive surgery is definitively made.
An incisional biopsy takes only a portion of the mole, so once the diagnosis is confirmed, further surgery is needed for a proper excision with good margins.
A core biopsy, however, is taken with a small device called a “punch,” which is a circular blade that takes a cylindrical core of skin ranging from 2 to 4 mm or more.
All of the above remove full thickness skin. The incisional and core biopsy should both include the border of the mole so the pathologist can compare normal skin to the lesion.
There is one more biopsy technique which must be mentioned: a shave biopsy, in which the surgeon takes a tangential cut through the mole. One serious shortcoming of shave biopsies is that often the blade cuts across the melanoma and its true depth and thickness cannot be determined.
This crucial information is provided to help you precisely plan surgery or provide a prognosis.
I feel that when melanoma is a possibility, a full thickness biopsy of the skin is critical. I avoid shave biopsies if melanoma is even a consideration.












